How to Identify Signs of Depression in Teens
A Practical Guide for Parents, Caregivers, and Educators
Understanding Teen Depression and Why Recognition Matters
Signs Of Depression
What If your child says “I hate Myself”
When someone says, “I hate myself,” it usually isn’t about literal hatred—it’s a signal of deep emotional distress. That phrase often reflects a mix of shame, frustration, and pain that the person may not know how to express more clearly.
One common reason is chronic self-criticism. People who set very high standards for themselves may feel like they’re constantly falling short. Over time, mistakes—big or small—can start to feel like proof that something is fundamentally wrong with them, rather than just part of being human.
Another factor is unresolved guilt or regret. If someone believes they’ve hurt others or made a serious mistake, they may internalize that event and let it define their entire identity. Instead of thinking “I did something bad,” the thought becomes “I am bad.”
Depression and anxiety also play a major role. These conditions can distort thinking, making negative thoughts feel absolute and permanent. The brain filters out positive evidence and amplates flaws, leading to a harsh, one-sided view of oneself.
There’s also the influence of past experiences, especially criticism, rejection, or trauma. If someone grew up hearing negative messages about themselves, those voices can become internalized and replayed as their own inner dialogue.
Importantly, saying “I hate myself” can sometimes be a way of asking for help without directly asking. It signals that the person is overwhelmed and struggling with their sense of worth.
While the feeling is real, it’s not a fixed truth. With support, reflection, and often professional help, people can learn to challenge those thoughts and build a more balanced, compassionate view of themselves.
What is teen depression? — defining clinical depression vs. moodiness
Adolescence is naturally a time of mood swings, identity changes, and social stress. However, clinical depression (major depressive disorder) is different from normal teenage moodiness. Clinical depression is a persistent condition that interferes with daily functioning — school, relationships, sleep, and safety — and typically lasts for weeks or months rather than hours or days.
Key differences:
- Moodiness: short-lived upset, predictable triggers, mood improves with time or distraction.
- Clinical depression: persistent low mood or irritability, loss of interest in activities, and changes in sleep or appetite that last most of the day, nearly every day for at least two weeks.
Why early recognition matters for youth outcomes
Early recognition matters because untreated teen depression:
- Increases risk for academic decline and substance use.
- Raises the risk of self-harm and suicide (suicide is a leading cause of death among adolescents).
- Can interfere with brain development, peer relationships, and long-term mental health.
Data points:
- The World Health Organization reports that depression is a leading cause of illness and disability among adolescents aged 10–19. [WHO: Adolescent mental health]
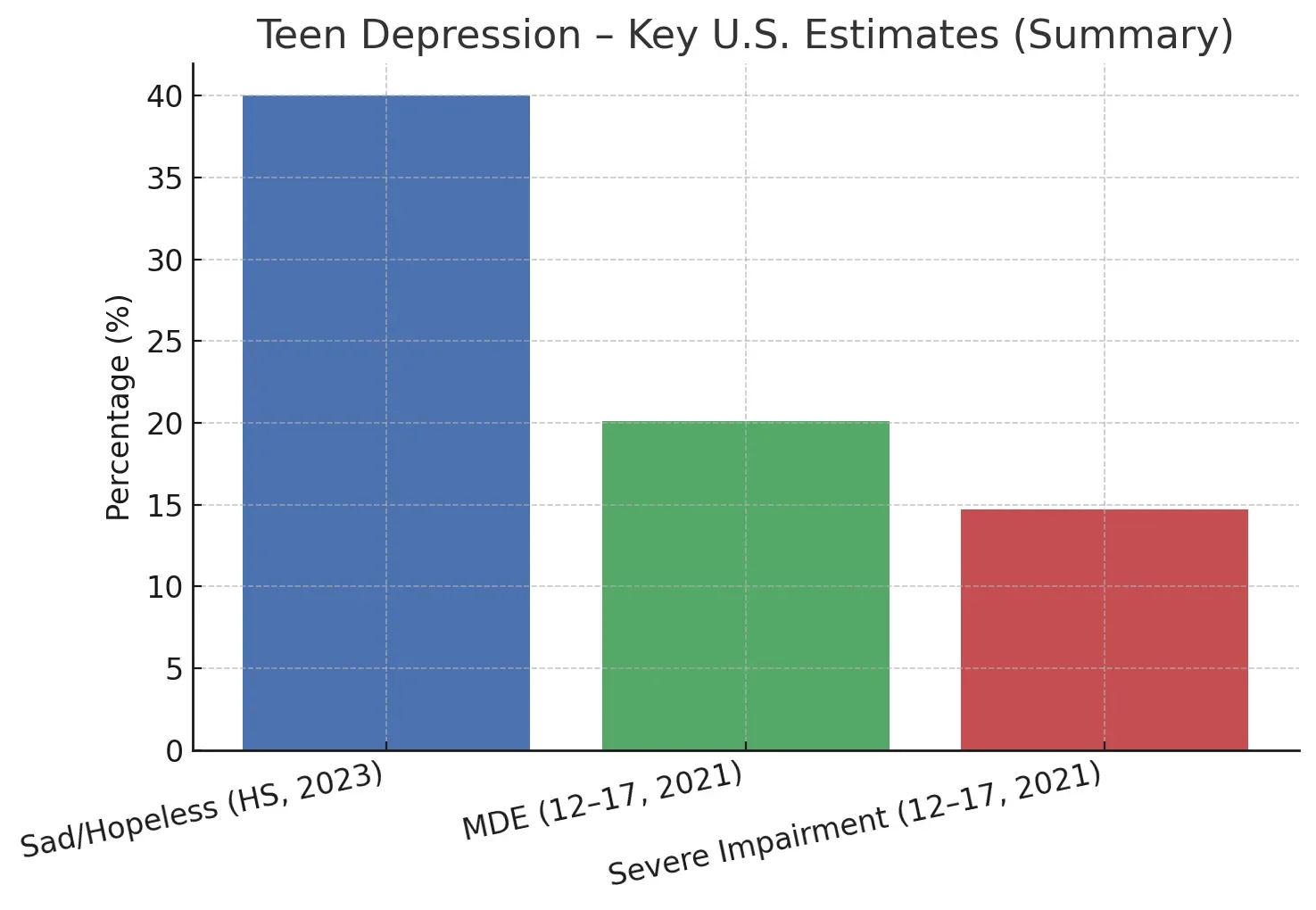
- In the U.S., the 2021 Youth Risk Behavior Surveillance System found that about 44% of high school students reported persistent feelings of sadness or hopelessness during 2021, with many also reporting suicidal thoughts. [CDC: YRBSS]
Common myths that delay help — linking to teen mental health awareness
- Myth: "They’ll grow out of it." — Many teens need treatment to recover.
- Myth: "Talking about suicide makes it worse." — Asking directly can reduce risk and improve safety.
- Myth: "Antidepressants change personality." — Medication can reduce symptoms and help therapy work better; side effects should be monitored.
Raising teen mental health awareness means replacing myths with facts so families and schools can act early.
Recognizing Emotional and Behavioral Teen Depression Symptoms
Clear recognition is the first step. Below are common teen depression symptoms framed so caregivers and educators can spot concerning patterns.
Emotional signs: persistent sadness, hopelessness, irritability
- Persistent feelings of sadness, tearfulness, or hopelessness lasting weeks
- Increased irritability, anger, or frequent emotional outbursts (especially in boys and younger teens)
- Loss of interest or pleasure in activities they once enjoyed (anhedonia)
- Statements like "What's the point?" or expressing worthlessness
Behavioral changes: withdrawal, declines in school performance, risky behavior
- Social withdrawal from friends and family, isolating in bedroom
- Drop in grades, reduced participation, missed assignments, or sudden school refusal
- Changes in hygiene or clothing choices (neglect or dramatic changes)
- Risky behaviors: increased substance use, reckless acts, or uncharacteristic rule-breaking
Cognitive and physical indicators: concentration problems, sleep/appetite changes, fatigue
- Difficulty concentrating, forgetfulness, indecision — affects schoolwork and daily tasks
- Noticeable weight loss or gain, or change in appetite
- Sleep changes: insomnia, early-morning awakening, or oversleeping
- Low energy, chronic fatigue, frequent complaints of physical aches without clear medical cause
LSI terms to watch for: adolescent mood disorder, teenage depression symptoms, low motivation, decreased concentration, somatic complaints.
Social and Environmental Clues: Contextual Signs in Teens
Depression doesn't occur in a vacuum. Look at relationships, school, and life events.
Peer and family relationship changes: isolation, conflict escalation
- Falling out with friends, being bullied, or withdrawing from family interactions
- Escalating conflict in the home — more arguments, avoidance of family meals, secretive behavior
- Expressing a sense of being trapped or misunderstood
School and extracurricular impact: absenteeism, drop in participation
- Increased absences or tardiness, leaving early from school frequently
- Disengagement from sports, clubs, or hobbies once important to the teen
- Teachers may report a change in participation, classroom conduct, or peer interactions
Life events and stressors that can trigger or worsen depression in youth
- Relationship breakups, LGBTQ+ stress, moving, parental separation/divorce, bereavement
- Academic pressure, college admissions stress, or financial instability at home
- Chronic illness, history of trauma, or ongoing bullying
> Depression often results from a combination of genetic vulnerability and environmental stressors. Recognizing both context and symptoms helps target support.
How to Talk to a Teen About Depression
The way you start the conversation matters. Aim for connection, not interrogation.
Preparing for the conversation: timing, setting, and tone
- Choose a calm, private time — not right before school or when emotions are high.
- Use a neutral setting: a quiet afternoon walk, car ride, or while doing a shared, low-pressure activity.
- Set a supportive tone: "I’ve noticed [specific behavior]. I’m concerned about you and want to help."
What to say and what to avoid: empathy, nonjudgmental language, listening strategies
What to say:
- "I’ve noticed you’ve seemed down lately, and I’m worried."
- "You’re not alone — I want to understand what you’re going through."
- Use open-ended prompts: "Can you tell me more about that?"
What to avoid:
- Dismissing phrases: "Everyone gets sad sometimes."
- Minimizing feelings: "It’s just a phase."
- Lectures or ultimatums that may shut down communication.
Listening strategies:
- Use reflective listening: repeat back what you heard to show understanding.
- Validate feelings: "That sounds really hard."
- Offer choices and collaborate: "Would you like me to help find someone to talk with, or would you prefer I sit with you while you make the call?"
When the teen resists: strategies to maintain connection and persistence
- Respect resistance but stay present: short check-ins, sending supportive texts, or leaving notes.
- Involve trusted adults: coaches, school counselors, or family friends the teen respects.
- Offer low-pressure resources: anonymous text lines, youth mental health apps, or information so they can take the lead when ready.
Practical Steps: When and How to Get Help
Knowing when to act and what options exist removes uncertainty.
Assessing severity and safety: self-harm or suicidal thoughts — immediate actions to take
Take any talk or sign of self-harm or suicide seriously:
- If there is immediate danger, call emergency services or take the teen to the nearest emergency department.
- In the U.S., call or text 988 for the Suicide & Crisis Lifeline, or use local emergency numbers overseas. [988 Lifeline]
- Remove access to means (medication, firearms, sharp objects) while arranging help.
Warning signs for urgent care:
- Talking about killing self or wanting to die
- Preparing for death (giving away possessions, saying goodbye)
- Sudden calm after a period of depression (may indicate a decision to act)
Counseling for teen depression: types of therapy, what to expect, and how to find a provider
Effective treatment often includes counseling — here are common, evidence-based therapies:
- Cognitive Behavioral Therapy (CBT): teaches skills to change negative thinking and behaviors.
- Interpersonal Therapy (IPT): focuses on relationships and role transitions.
- Dialectical Behavior Therapy (DBT) skills (for intense emotion regulation and self-harm behaviors).
- Family Therapy: addresses family dynamics and communication patterns.
What to expect:
- An intake assessment, safety planning, and a treatment plan with goals.
- Regular sessions (weekly or biweekly) for several months, with progress reviews.
- Collaboration with pediatricians or psychiatrists if medication is considered.
How to find a provider:
- Use your insurance’s mental health directory, [SAMHSA’s treatment locator](https://findtreatment.samhsa.gov/), or local pediatric/mental health clinics.
- Ask school counselors or pediatricians for recommendations.
- Look for clinicians who list adolescent experience and evidence-based approaches.
Medication, school accommodations, and coordinated care:
working with healthcare and school systems
Medication:
- Antidepressants (SSRIs) may be prescribed for moderate to severe depression; monitoring for side effects is essential.
- Decisions should be made jointly by caregivers, teens (when appropriate), and prescribers.
School accommodations:
- 504 Plans and Individualized Education Programs (IEPs) can provide classroom accommodations, extended deadlines, excused absences for treatment, or counseling time. In the U.S., school counselors and special education teams can start this process.
Coordinated care:
- Effective care often involves coordination among family, therapists, primary care providers, and schools. Regular communication (with the teen’s consent) keeps supports aligned.
Building Ongoing Support and Promoting Teen Mental Health Awareness
Recovery and resilience are built over time with supportive routines and systems.
Home strategies: routines, communication, and healthy coping skills
- Maintain consistent sleep and meal routines; encourage gentle physical activity.
- Model emotional regulation and healthy coping (mindfulness, journaling, breathing exercises).
- Create predictable family check-ins and maintain open lines of communication.
Simple coping skills to teach:
- Deep breathing (4-4-6 pattern), grounding techniques (5-4-3-2-1), short walks, scheduling pleasant activities.
School and community roles: counseling services, peer support, and awareness programs
- Schools can host mental health education, peer-support programs, and on-site counseling.
- Community centers, faith groups, and youth organizations often run resilience-building activities and mentorship programs.
- Awareness initiatives reduce stigma and encourage help-seeking.
Long-term monitoring and relapse prevention: check-ins, booster sessions, and family involvement
- Schedule routine check-ins after symptoms improve; relapse is common and treatable.
- Booster therapy sessions can reinforce coping skills.
- Keep a simple monitoring plan for early warning signs (sleep, interest level, school performance).
> Mental health is a chronic-care model for many: treat, monitor, and adjust as needed.
Conclusion: Action Steps and Resources
Quick checklist for parents and caregivers to spot teen depression symptoms and seek help
- Look for persistent mood changes (2+ weeks), loss of interest, and functional decline.
- Ask direct, empathetic questions about mood and safety.
- If safety is immediate, call emergency services or a crisis line (U.S. 988).
- Seek a mental health assessment from pediatrician, school counselor, or licensed therapist.
- Arrange counseling and consider coordination with school for accommodations.
How to make a simple safety and support plan for an adolescent in need
Use this basic template and adapt it with the teen’s input:
Safety & Support Plan
1) Warning signs: (what we notice) _________________________
2) Coping strategies the teen can use: ______________________
3) People to contact for support (family/friend): Name & phone____
4) Professional contacts: Therapist/Doctor: Name & number_______
5) Steps if suicidal or unsafe: Call 988 / go to ER / call 911
6) Remove/restrict access to means: list items to secure/remove_____
7) Date to review plan: __________________
Teen Statistics
Recommended resources: hotlines, national organizations, and guides for counseling for teen depression
- U.S. Suicide & Crisis Lifeline (988)
- World Health Organization — Adolescent mental health facts
- Centers for Disease Control and Prevention — Youth Risk Behavior Surveillance System
- National Institute of Mental Health — Depression in Children and Adolescents
- National Alliance on Mental Illness (NAMI) — Teen resources
- SAMHSA Treatment Locator — Action steps (call to action)
- If you suspect a teen is depressed, start with a calm, caring conversation this week.
- If there's any talk or sign of self-harm, call your local emergency number or a crisis hotline immediately.
- Share this guide with another caregiver, teacher, or coach to promote teen mental health awareness in your community.
Supporting a depressed teen is a process — with early recognition, compassionate conversation, and timely treatment (including counseling for teen depression when indicated), most adolescents recover and regain their wellbeing. If you need help right now, reach out to a local crisis resource or your teen’s health care provider.