Understanding Child Behavioral Issues
Understanding Child Behavioral Issues: Signs and Interventions
Introduction: Why Understanding Child Behavioral Issues Matters
The aim of this article and who it’s for
This guide is for parents, caregivers, teachers, and frontline professionals who want practical, evidence-informed help with child behavior. Whether you notice early warning signs or want long-term strategies, this article shows how to spot child behavior problems. It also outlines intervention and counseling options. It balances clinical perspectives with everyday tactics so you can take immediate action and plan for sustained improvement.
Quick overview of common terms (behavioral issues, behavior management techniques children)
- Behavioral issues: patterns of acting out, withdrawal, or difficulty regulating emotions that interfere with learning, relationships, or safety.
- Behavior management techniques children: concrete practices (reinforcement systems, routines, limits) used to modify and support child behavior.
Interventions for child behavior: structured programs or targeted strategies (therapy, parent training, school plans) that reduce problem behaviors. They also teach better options.
How early recognition improves outcomes (recognizing child behavioral problems)
Early recognition leads to earlier support and better outcomes. For example, early behavior support and parent training can stop problems before they start. It can help children do better in school. It can also reduce the need for intensive services later. According to the U.S. Centers for Disease Control and Prevention (CDC), 1 in 6 children aged 2–8 years have a diagnosed mental, behavioral, or developmental condition — early attention matters. [CDC: Child Development and Behavior]
Recognizing the Signs: Child Behavioral Issues Signs to Watch For
Identifying child behavioral issues signs early helps you decide whether to monitor, adapt your approach, or seek formal help. Below are common indicators across emotional, social, academic, and developmental domains.
Emotional and social indicators
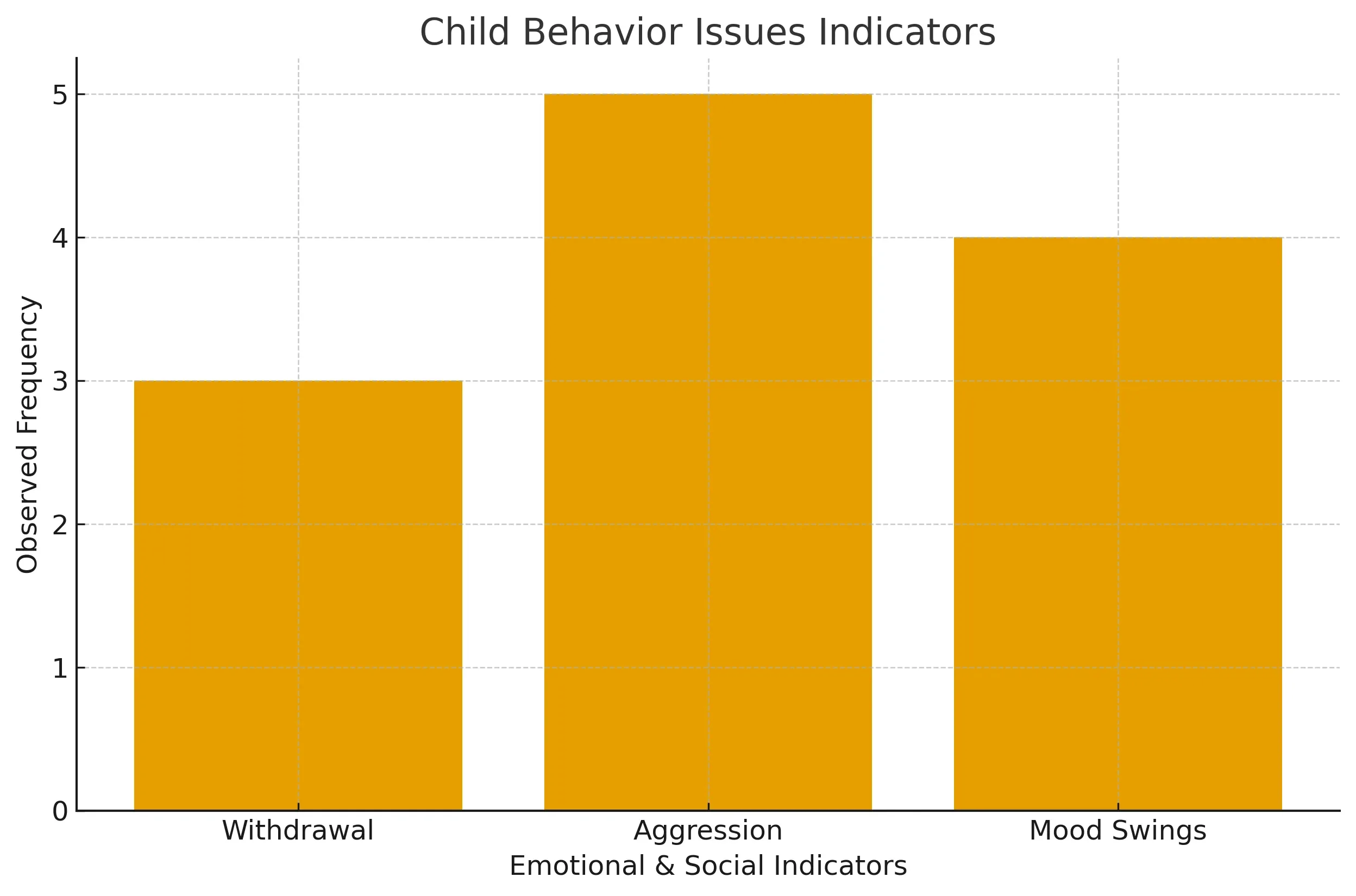
Emotional and social indicators (withdrawal, aggression, mood swings)
- Frequent temper outbursts that are out of proportion to the situation
- Persistent irritability, sadness, or anxiety
- Withdrawal from peers or refusal to participate in age-appropriate activities
- Aggression toward peers, caregivers, or animals
- Trouble making or keeping friends, bullying behavior, or being bullied
> Tip: If emotional symptoms interfere with daily functioning for weeks or months, treat them as significant and discuss them with a pediatrician or mental health professional.
Academic and attention-related signs (inattention, declining school performance)
- Difficulty paying attention in class, incomplete schoolwork, careless mistakes
- A sudden drop in grades or motivation without obvious academic difficulty
- Frequent complaints from teachers about classroom behavior or disruptions
- Trouble following instructions or staying on task despite age-appropriate supports
Statistics: ADHD affects about 8–10% of U.S. children, based on the study and diagnostic criteria. Accurate assessment helps tailor interventions.
Behavioral patterns by age and severity
(how to distinguish typical behavior from problems)
- Toddlers: Tantrums are common, but persistent aggression or inability to soothe may signal concerns.
- Preschool: High impulsivity is typical, but extreme defiance and safety risks call for evaluation.
- School-age: Problems that impair learning, peer relationships, or family functioning are not just "growing pains."
- Adolescents: Substance use, running away, or sustained risky behaviors require immediate attention.
Recognizing child behavioral problems means distinguishing developmentally typical behavior from patterns that persist or worsen and cause impairment.
Causes and Risk Factors Behind Behavioral Problems
Understanding causes helps choose the right approaches to child behavior issues. Most behavioral problems arise from a mix of biological, environmental, and psychological influences.
Biological and developmental contributors (neurodiversity, genetics)
- Neurodevelopmental conditions such as ADHD or autism spectrum disorder (ASD) can underlie behavioral differences.
- Genetic predispositions and temperament affect stress response and impulse control.
- Medical issues (sleep disorders, hearing/vision problems, chronic illness) can mimic or worsen behavioral symptoms.
Environmental and family influences (stress, trauma, inconsistent discipline)
- Family stress, parental mental health issues, inconsistent discipline, and exposure to violence or instability increase risk.
- Trauma or adverse childhood experiences often manifest as emotional dysregulation and behavior problems.
- Socioeconomic factors, community violence, or school environment can compound risks.
Co-occurring mental health conditions and medical factors
- Anxiety, depression, oppositional defiant disorder (ODD), and conduct disorder can co-occur with behavioral problems.
- Substance use or neurological conditions require evaluation and integrated care.
> Good practice: A functional assessment (what triggers and maintains a behavior) helps tailor interventions rather than using a one-size-fits-all approach.
Approaches to Child Behavior Issues: Frameworks and Theories
Several evidence-informed frameworks guide interventions for child behavior. Use these as lenses to choose specific techniques.
Positive behavior support and reinforcement strategies
- Emphasizes proactive changes to environment, predictable routines, and reinforcement of desired behavior.
- Uses rewards, token economies, and natural consequences to encourage positive behavior.
- Works well in homes, classrooms, and clinics.
Cognitive-behavioral and family systems approaches
- Cognitive-behavioral therapy (CBT) teaches children skills to manage thoughts, emotions, and behaviors.
- Family systems therapy addresses relational patterns, parental responses, and communication.
- Parent-Child Interaction Therapy (PCIT) blends parenting coaching with child-focused play therapy for young children.
School-based and community-centered approaches
- Individualized Education Programs (IEPs) and 504 Plans (U.S.) provide academic accommodations.
- Multi-tiered Systems of Support (MTSS) and Positive Behavioral Interventions and Supports (PBIS) are school-wide frameworks.
- Community programs, after-school activities, and mentoring can reduce risk and enhance protective factors.
These approaches to child behavior issues guide the design of targeted interventions for child behavior in different settings.
Interventions for Child Behavior: Practical Strategies and Programs
This section moves from theory to concrete tools you can apply immediately and over time.
Short-term strategies for immediate behavior management
(de-escalation, consistent routines)
- Stay calm and use a neutral voice; mirror calm behavior to de-escalate.
- Remove the child from triggers when safety is at risk.
- Use simple, clear instructions and one-step directions for young children.
- Maintain consistent daily routines—mealtimes, sleep, homework, and screen limits.
Immediate tactics:
- Offer choices (limited and specific): "Do you want to put your shoes on or your jacket first?"
- Use brief time-outs as a reset (explain purpose ahead of time).
- Praise specific behavior: "I like how you used your words to ask for a turn."
Long-term interventions and structured programs
(parent training, behavior plans)
- Parent management training (PMT) teaches consistent reinforcement and clear limits; it has strong evidence for reducing disruptive behavior.
- School behavior plans and functional behavior assessments (FBA) identify triggers and replacement behaviors.
- Intensive outpatient programs and day-treatment options for severe cases.
Programs to consider:
- Parent-Child Interaction Therapy (PCIT)
- Triple P (Positive Parenting Program)
- Behavioral parent training and CBT for older children
Behavior management techniques children can use
(reward systems, clear expectations)
- Reward charts and token economies tied to immediate, visible rewards.
- Social stories and role-play for children with ASD or social difficulties.
- Self-monitoring checklists for older children and adolescents to track goals and progress.
Example reward system:
- Short-term: 1 point per completed homework; 10 points = special activity.
- Ensure rewards are meaningful and age-appropriate.
> Interventions for child behavior work best when they are consistent, measurable, and reinforced across home and school.
Child Behavior Counseling Options: When and Where to Seek Help
Knowing when to seek professional help and which provider fits your needs reduces delay in effective care.
Types of professionals and services
(pediatricians, child psychologists, behavioral therapists)
- Pediatrician or GP: first contact for screening, medical assessment, and referrals.
- Child psychologist/psychiatrist: diagnostics, therapy, and medication management if needed.
- Licensed behavioral therapists and applied behavior analysts (ABA) for ASD-related behavior supports.
- School counselor or school psychologist for in-school interventions and plans.
What to expect in counseling and therapeutic approaches
(individual, family, group therapy)
- Assessment: interviews, rating scales, and observation. Tools like the Vanderbilt Assessment Scale or Strengths and Difficulties Questionnaire (SDQ) are commonly used.
- Therapy: CBT, parent training, family therapy, social skills groups, or play therapy depending on age and diagnosis.
- Medication: sometimes recommended for ADHD, severe anxiety, or mood disorders; typically combined with behavioral interventions.
How to choose the right program and access community resources
- Ask about evidence base: “Is this program supported by randomized trials or reputable guidelines?”
- Check credentials and experience with your child’s age and condition.
- Use local resources: school special needs teams, public health clinics, and national directories.
- In the U.S.: contact the [Substance Abuse and Mental Health Services Administration (SAMHSA)] for treatment locators.
- In the U.K.: consult the [NHS] and local Child and Adolescent Mental Health Services (CAMHS).
Include “child behavior counseling options” in your search and compare services based on approach, cost, accessibility, and cultural fit.
Supporting Parents and Caregivers: How to Help Child Behavior at Home
Parents and caregivers are central to successful outcomes. Practical home strategies make a big difference.
Creating consistent routines and setting boundaries
- Create predictable daily schedules for sleep, meals, homework, and play.
- Use clear, simple rules and consistently enforced consequences.
- Plan ahead for transitions (use timers, alerts, or rehearsal for upcoming changes).
Communication skills and emotional coaching for parents
- Label feelings: “I can see you’re frustrated because your toy broke.”
- Teach coping skills: deep breathing, counting, or “calm-down” corners.
- Use active listening and reflective statements: “You’re upset because you wanted to play longer.”
Collaborating with schools and professionals for coordinated care
- Share behavior plans between home and school to ensure a consistent approach.
- Request teacher observations and regular check-ins.
- Engage in multidisciplinary meetings (teachers, therapists, pediatrician) for coordinated care.
> How to help child behavior: start small, be consistent, and involve the child in goal-setting to build ownership.
Case Examples and Practical Worksheets
Brief anonymized case studies illustrating common interventions
Case 1 — Luke, age 7: Frequent classroom disruptions. Solution: FBA conducted; implemented a token economy at school and home. After 8 weeks, disruptions decreased by 60% and homework completion improved.
Case 2 — Maya, age 4: Aggressive tantrums at transitions. Solution: Introduced visual schedules, a 2-minute countdown before transition, and parent coaching in positive reinforcement. Tantrums reduced to manageable levels in 6 weeks.
Simple templates: behavior plan, communication script, progress tracker
Behavior Plan Template:
Goal: (e.g., Reduce hitting at home)
Target behavior: (e.g., Hitting others)
Antecedent: (triggers)
Replacement behavior: (e.g., Use words, seek adult)
Reinforcement: (e.g., 1 point per incident-free day)
Consequence: (e.g., Lose screen time for hitting)
Review date: (e.g., 4 weeks)
Communication Script (for parents):
- Parent: “I see you’re upset because [reason].”
- Child: (pause to respond)
- Parent: “You can tell me you’re angry, or use your calm-down tool. When you’re ready, we’ll [alternative action].”
Progress Tracker (weekly):
- Monday to Friday checklist: Target behaviors observed (Yes/No), Points earned, Notes.
Tips for adapting plans to different ages and needs
- Younger children: use visuals, immediate rewards, and play-based coaching.
- School-age: involve teachers, use token economies with specific school privileges.
- Adolescents: negotiate goals, use natural consequences, and incorporate technology for reminders.
Conclusion: Next Steps and Resources
Summary of key signs, approaches, and intervention options
Recognizing child behavioral problems early — emotional withdrawal, aggression, attention issues, or academic decline — allows for timely, tailored interventions. Approaches range from positive behavior support and parent training to CBT and school-based programs. Practical, consistent behavior management techniques children can use include reward systems, clear expectations, and routines. When concerns persist or impair life functioning, explore child behavior counseling options with pediatricians and mental health professionals.
Actionable first steps for parents and educators
(when to monitor vs. when to seek help)
- Monitor for 2–4 weeks if behavior is mild and context-specific; implement consistent routines and simple reward systems.
- Seek professional advice if behavior:
- Threatens safety (self-harm, aggression)
- Persistently impairs school or family functioning
- Is accompanied by regression in skills or extreme mood changes
Further resources and recommended reading, hotlines, and professional directories
- CDC — Child Development & Mental Health:
- American Academy of Pediatrics (AAP) guidance:
- NHS — Mental health and behavior in children:
- U.S. crisis line: Dial 988 for immediate mental health crisis help
- Childhelp National Child Abuse Hotline: 1-800-4-A-CHILD (1-800-422-4453) — > “Early help, consistent supports, and coordinated care make a real difference — you don’t have to do this alone.”
Call to action:
- If you're a caregiver or educator who recognizes child behavioral issues signs in a child you care for, start by documenting specific behaviors for two weeks, implement one simple behavior management technique, and schedule a check-in with your pediatrician or school counselor. If you're ready for professional help, search “child behavior counseling options” in your area and request an intake evaluation.