Nutrition's Role in Mental Health
Nutrition's Role in Mental Health: A Comprehensive Guide to Eating for Mental Health Improvement
Introduction: Why Nutrition and Mental Health Matter
The link between food and mood: how nutrition affects mental health
If you've ever felt "hungry" or more irritable after a sugar-heavy snack, you know instinctively that food can change mood. Research now supports that intuition: what we eat influences brain chemistry, inflammation, and the gut microbiome — all of which shape emotional states. Learning about *how nutrition affects mental health helps you make dietary changes for better mental health that are realistic and effective.
"Nutrition is not a cure-all, but it is a powerful modifiable factor that can support mental wellness."
Scope and goals: what readers will learn about dietary changes for better mental health
This guide explains the science linking nutrition and mental health, lists key nutrients and foods for emotional wellness, compares beneficial dietary patterns, and gives practical, everyday strategies for eating for mental health improvement. You’ll find quick meals, snack ideas, mindful-eating tips, guidance on supplements, and a sample weekly menu to get started.
How to use this guide: who benefits from nutrition tips for emotional wellness
- Adults managing mild-to-moderate mood symptoms
- Caregivers and parents seeking food-based support for children or adolescents
- Older adults and people with chronic health conditions who want better mood and cognition
- Anyone curious about the *impact of diet on mood* and wanting doable dietary changes
Use sections relevant to your situation, try simple swaps first, and consult a clinician for moderate or severe mental health conditions.
The Science Behind Food for Mental Well-Being
Brain chemistry and nutrients: neurotransmitters, inflammation, and the gut-brain axis
Food provides building blocks and cofactors for neurotransmitters (e.g., serotonin, dopamine), affects systemic inflammation, and feeds gut bacteria that communicate with the brain — the so-called *gut-brain axis*. Examples:
- Amino acids like tryptophan are precursors for serotonin.
- B vitamins (B6, B9/folate, B12) are essential for neurotransmitter synthesis and one-carbon metabolism.
- Omega-3 fatty acids (EPA, DHA) integrate into neuronal membranes and modulate signaling and inflammation.
- Dietary fiber and probiotics help maintain a diverse microbiome that produces metabolites (short-chain fatty acids) influencing brain function.
Evidence overview: research on the impact of diet on mood and mental disorders
Clinical evidence is growing. Key findings include:
- The SMILES randomized controlled trial (2017) found that a dietary intervention modeled on Mediterranean principles produced clinically significant improvements in adults with major depression compared with social support alone (Jacka et al.)
- Population studies and meta-analyses link higher adherence to Mediterranean-style or whole-food patterns with lower risk of depression and better mental health outcomes.
- Evidence for specific supplements is mixed: omega-3s (especially EPA) show promise in some meta-analyses; vitamin D and B-vitamin supplementation may help when a deficiency is present. See NIH resources and reviews for nuance.
For global context: depression affects an estimated 280 million people worldwide and is a leading cause of disability (World Health Organization). [WHO depression fact sheet]
Common misconceptions: separating marketing claims from science about nutrition and mental health
- Myth: One "superfood" will fix depression. Reality: no single food cures mental illness. Benefits come from overall patterns and consistent habits.
- Myth: Supplements always help. Reality: Supplements may help if you have a documented deficiency; otherwise evidence varies and quality control is inconsistent.
- Myth: Carbs are bad for mood. Reality: Refined carbs can worsen mood swings and inflammation; but whole grains and fiber-rich carbs support stable blood sugar and gut health.
Key Nutrients and Foods That Support Emotional Wellness
Omega-3s, B vitamins, vitamin D, magnesium and their roles in mood regulation
- Omega-3 fatty acids (EPA and DHA): Found in fatty fish (salmon, sardines), flaxseed, chia. Studies suggest EPA-rich formulations can reduce depressive symptoms for some people. Aim for 1–2 servings of fatty fish per week or discuss supplementation if diet is low in fish.
- B vitamins (B6, B9/folate, B12): Critical for neurotransmitter synthesis. Good sources include leafy greens, legumes, fortified cereals, eggs, dairy, and lean meats. Low folate/B12 associates with depressive symptoms; supplementation may help in deficiency.
- Vitamin D: Low vitamin D levels correlate with higher depression risk in some studies. Get regular sun exposure, dietary sources (fortified milk, fatty fish), and test if deficiency is suspected. [NIH vitamin D fact sheet]
- Magnesium: Supports nervous system function; low magnesium can worsen anxiety and sleep. Sources: nuts, seeds, whole grains, legumes, dark leafy greens.
Gut-friendly choices: probiotics, fiber, and food for mental well-being via the microbiome
- Fermented foods (yogurt with live cultures, kefir, sauerkraut, kimchi, miso) can support microbial diversity.
- Dietary fiber from whole grains, fruits, vegetables, and legumes feeds beneficial bacteria that produce short-chain fatty acids linked to improved brain function.
- Emerging research on "psychobiotics" is promising but preliminary — eating a variety of fiber-rich plant foods is a practical first step.
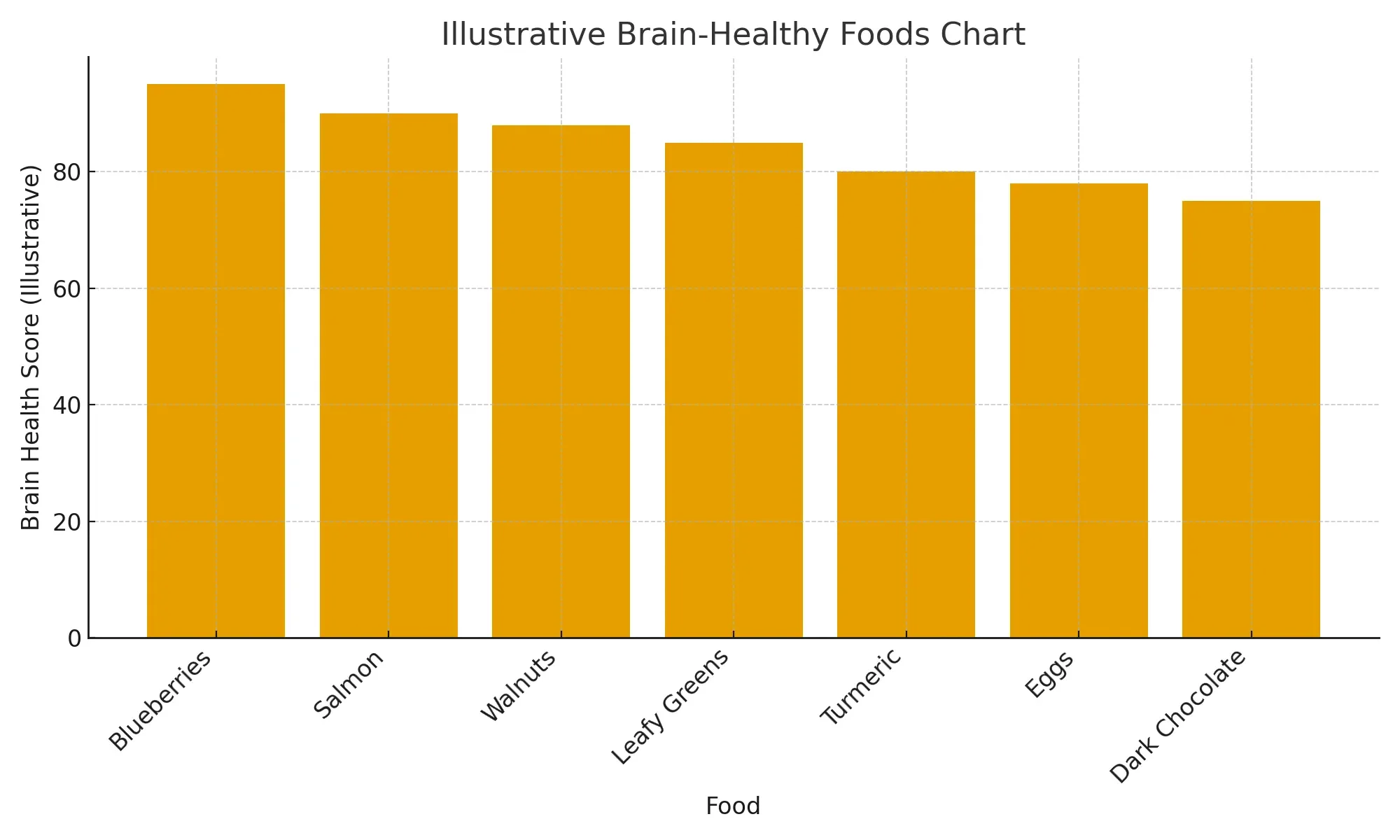
Antioxidants and phytonutrients: how plant-based foods protect brain health
- Fruits, vegetables, berries, nuts, seeds, tea, and spices contain polyphenols and antioxidants that reduce oxidative stress and inflammation in the brain.
- Blueberries, leafy greens, and colorful vegetables rank high in neuroprotective phytochemicals.
- A diet rich in plant-based foods correlates with better cognitive function and lower rates of mood disorders.
Dietary Patterns and Practical Strategies for Better Mental Health
Mediterranean, whole-food, and anti-inflammatory diets: patterns linked to improved mood
1. Overview
Diet is increasingly recognized as a modifiable determinant of mental health. Evidence from nutritional psychiatry indicates that specific dietary patterns can influence inflammation, neuroplasticity, neurotransmitter synthesis, and the gut–brain axis—factors that collectively impact mood, cognition, and resilience to psychological stress.
2. Evidence-Based Dietary Patterns for Mental Health
Mediterranean Diet
Considered the most studied and validated diet for supporting mental well-being.
High in: fruits, vegetables, nuts, legumes, whole grains, olive oil, fish
Moderate in: fermented dairy, poultry
Low in: processed foods, refined sugars, red meats
Benefits:
Reduced risk of depression and anxiety
Lower systemic inflammation
Enhanced cognitive performance and reduced risk of dementia
MIND Diet (Mediterranean–DASH Intervention for Neurodegenerative Delay)
Designed specifically to protect cognitive function.
Emphasizes leafy greens, berries, nuts, beans, whole grains, olive oil, fish
Benefits:Slower cognitive decline
Lower Alzheimer’s disease risk
Anti-Inflammatory Diet
Targets chronic inflammation, which is strongly linked to mood disorders.
Includes fatty fish, turmeric, ginger, berries, nuts, seeds, leafy greens
Benefits:Improved mood stability
Reduced anxiety symptoms
Traditional and Whole-Food Diets
Indigenous, Okinawan, and Nordic diets also correlate with better mental health outcomes through reliance on unprocessed, nutrient-dense foods.
3. Critical Nutrients for Mental Health
Omega-3 Fatty Acids (EPA & DHA)
Found in: salmon, sardines, mackerel, walnuts, flaxseed
Role: Supports neuronal membrane fluidity, serotonin signaling, and anti-inflammatory pathways.
B Vitamins (especially B6, B9, B12)
Found in: leafy greens, beans, whole grains, eggs, poultry
Role: Essential for neurotransmitter synthesis (serotonin, dopamine).
Magnesium
Found in: nuts, seeds, whole grains, legumes
Role: Regulates stress response, relaxation, and sleep.
Zinc
Found in: seafood, nuts, seeds
Role: Neurogenesis and neurotransmission.
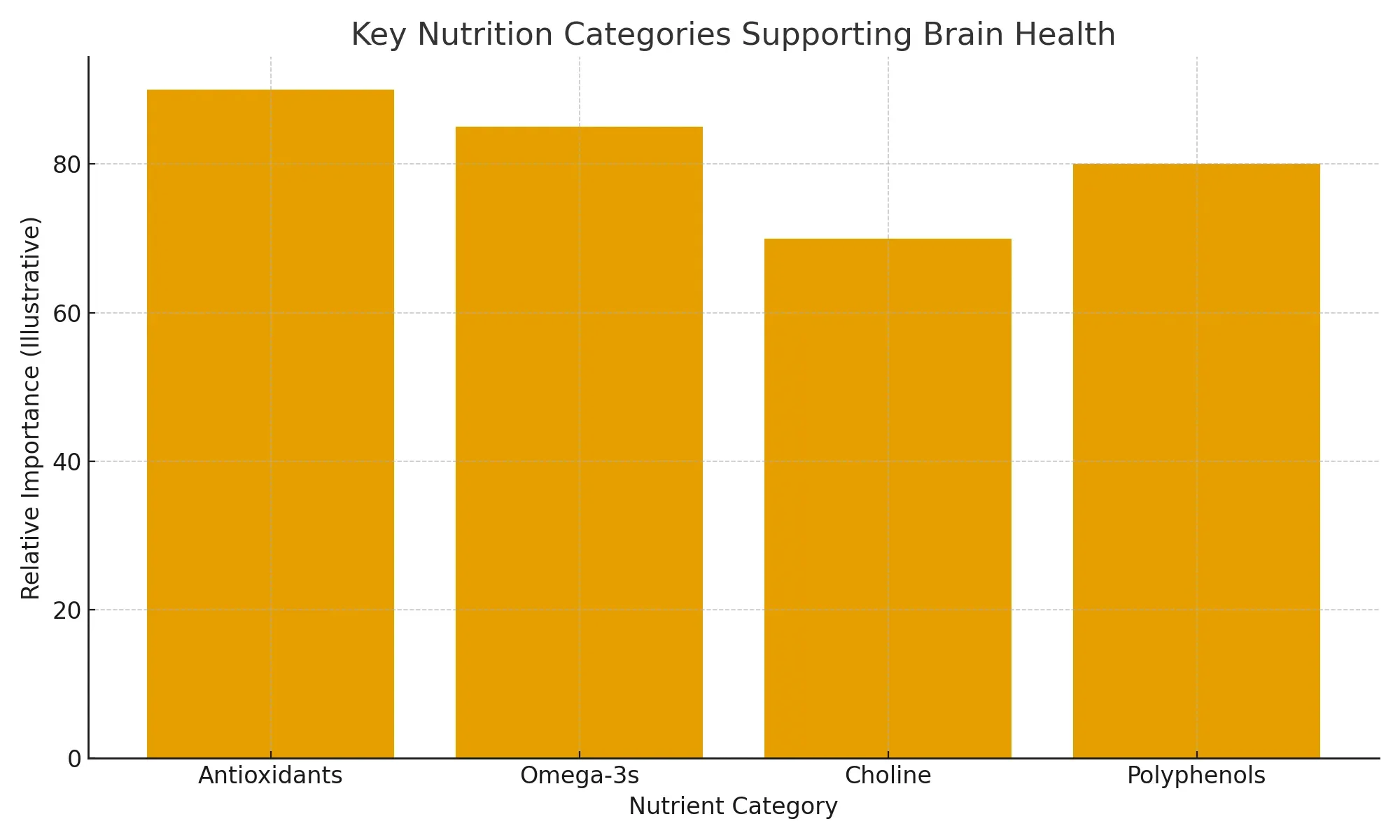
Antioxidants (including Polyphenols)
Found in: berries, dark chocolate, green tea, colorful vegetables
Role: Reduce oxidative stress linked to depression and cognitive decline.
Choline
Found in: eggs, fish, poultry
Role: Precursor for acetylcholine; supports memory and attention.
4. The Gut–Brain Axis and Mental Health
Key Mechanisms
Gut bacteria synthesize neurotransmitters (GABA, serotonin)
Diet influences inflammation and immune signaling
Fiber and fermented foods promote microbial diversity
Supportive Foods
Probiotics: yogurt, kefir, kimchi, sauerkraut
Prebiotics: onions, garlic, oats, bananas, beans
Impact: Improved mood regulation, stress resilience, and cognitive clarity.
5. Practical Strategies for Implementation
Build a Mental-Health-Supportive Plate
Half vegetables
One-quarter whole grains
One-quarter lean proteins (preferably fish or plant-based)
Add healthy fats: olive oil, nuts, seeds
Reduce Foods Linked to Poor Mental Health
Ultra-processed snacks
Added sugars
Refined carbohydrates
Excess alcohol
Artificial trans fats
Timing and Eating Patterns
Choose consistent meal intervals to stabilize blood sugar
Pair protein + fiber every meal for energy and mood stability
Consider time-restricted eating if appropriate and medically safe
Hydration Strategy
Aim for consistent fluid intake
Prioritize water and unsweetened teas
Dehydration is linked to mood volatility and impaired concentration
Supplements (when food intake is insufficient)
Omega-3 (EPA-dominant
Vitamin D3
Magnesium glycinate
B-complex
Always consider professional guidance and testing.
6. Behavioral and Lifestyle Integration
Mindful Eating
Slow, deliberate meals reduce stress and improve digestion
Helps tune into hunger and fullness cues
Meal Planning
Prepare three days of meals at a time
Stock staples: beans, nuts, frozen vegetables, eggs, whole grains
Stress-Resilient Eating
Avoid stress-driven snacking
Build rituals: herbal tea, structured meal times, distraction-free eating
Sleep and Exercise Synergy
Diet interacts with:
Sleep quality
Physical activity
Light exposure
Optimizing these magnifies nutritional benefits.
7. Summary
A dietary approach to better mental health focuses on:
Whole-food, plant-forward patterns
Healthy fats, sufficient protein, and antioxidant-rich produce
Reducing inflammatory and processed foods
Supporting gut health through fiber and fermented foods
Collectively, these strategies strengthen mood regulation, emotional resilience, and cognitive performance.Simple dietary changes for better mental health: swap ideas and small daily habits
Make gradual swaps rather than all-or-nothing changes. Examples:
- Swap sugary breakfast cereal for oatmeal topped with nuts and berries.
- Replace soda with sparkling water and a squeeze of lemon or herbal tea.
- Add a serving of oily fish or a can of sardines twice a week.
- Choose whole fruits over fruit juices to increase fiber and reduce glycemic load.
- Include a leafy green or vegetable at every lunch and dinner.
Each small change supports *eating for mental health improvement* without overwhelming your routine.
Meal planning and timing: eating for mental health improvement through routine and balance
- Aim for balanced meals with protein, fiber-rich carbs, and healthy fats to stabilize blood sugar and mood.
- Regular meal timing supports circadian rhythms — inconsistent eating can disrupt sleep and mood.
- Plan 2–3 simple, repeatable breakfasts and lunches you enjoy; rotate dinners weekly. Batch-cook legumes, grains, and roasted veggies for quick assembly.
Nutrition Tips for Emotional Wellness in Real Life
Quick, nutrient-dense meals and snacks for busy days (breakfasts, lunches, snacks)
Breakfast ideas:
- Greek yogurt with berries, walnuts, and a drizzle of honey.
- Overnight oats with chia seeds, banana, and almond butter.
- Scrambled eggs with spinach and whole-grain toast.
Lunch ideas:
- Quinoa salad with canned salmon, cucumber, tomatoes, olive oil, lemon.
- Lentil soup with carrots, celery, and a side of whole-grain bread.
- Whole-grain wrap with hummus, roasted vegetables, and salad greens.
Snacks:
- Apple slices with peanut butter.
- Handful of almonds and a piece of dark chocolate (70% cocoa).
- Kefir or probiotic yogurt and a small banana.
Managing cravings, stress-eating and emotional triggers with mindful eating techniques
- Pause for a 5–10 minute breath before eating when stressed: assess hunger vs. habit.
- Eat without screens to notice satiety cues.
- Keep healthy, portion-controlled snacks accessible; remove trigger foods from easy reach.
- Practice the "HALT" check: Are you Hungry, Angry, Lonely, or Tired? This helps identify emotional eating triggers.
Supplements, safety and when to consult a professional about nutrition and mental health
- Supplements can help when nutrient deficiencies exist (e.g., vitamin D, B12, iron). Get blood tests when possible.
- Omega-3 supplements should prioritize EPA content; discuss dosage with your clinician, especially if you take blood thinners.
- Consult a registered dietitian or your primary care provider if you have:
- Persistent mood symptoms
- Multiple nutrient deficiencies
- Eating disorders, medical conditions, or complex medication regimens
Special Considerations and Populations
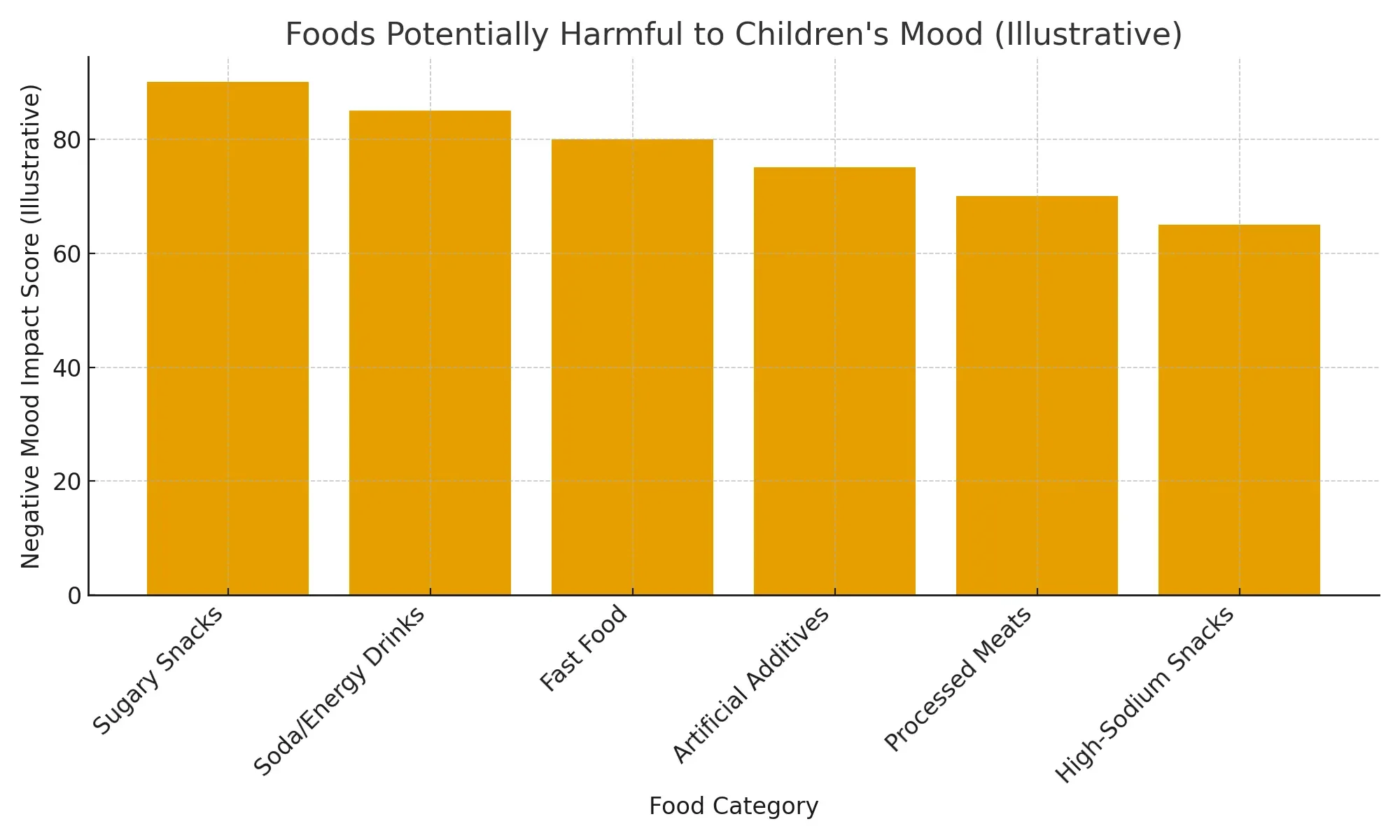
Bad Mood Foods For Kids Chart
Children, adolescents and students: tailored nutrition strategies for mood and cognition
- Promote regular meals and snacks to stabilize blood sugar and concentration.
- Encourage varied breakfasts (protein + fiber) and pack nutrient-dense school lunches: whole grains, lean protein, fruit, and vegetables.
- Limit highly processed snack foods and sugary beverages that can worsen attention and mood.
- In adolescents, ensure adequate iron, B12, and vitamin D; screen when symptoms appear.
Older adults and metabolic or chronic conditions: adapting food for mental well-being
- Older adults may need nutrient-dense yet easy-to-chew options: stews, smoothies with added greens and nut butter, soft-cooked fish.
- Address common deficiencies (B12, vitamin D) and polypharmacy interactions.
- Manage chronic disease (diabetes, cardiovascular disease) with anti-inflammatory dietary patterns that also support mood.
Cultural, economic and accessibility factors: realistic food for mental well-being solutions
- Affordable, nutrient-dense choices: canned fish (sardines, salmon), beans and lentils, frozen vegetables, oats, and eggs.
- Culturally relevant foods can provide the same nutrients: e.g., chickpea stews, rice-and-bean dishes, fermented foods from diverse cuisines.
- Community resources: food banks, SNAP benefits (U.S.), local community gardens, and cooking classes can improve access.
Implementing Sustainable Dietary Changes for Long-Term Mood Benefits
Setting realistic goals and tracking progress: turning nutrition tips for emotional wellness into habits
- Start small: choose 1–2 changes for 2 weeks (e.g., add one vegetable at dinner, swap soda for water).
- Track progress with a simple mood journal (date, sleep, what you ate, mood rating 1–10). Look for patterns over 2–4 weeks.
- Use SMART goals: Specific, Measurable, Achievable, Relevant, Time-bound. Example: "Eat two servings of oily fish per week for one month."
Working with clinicians: combining dietary changes for better mental health with therapy and medication
- Nutrition is an adjunct — not a replacement — for evidence-based therapy and medication when indicated.
- Tell your mental health provider about major dietary changes and supplements to avoid interactions.
- Consider collaborative care: behavioral health clinicians and registered dietitians can coordinate plans for best outcomes.
Recipes and weekly sample menu: concrete examples of eating for mental health improvement
Below is a simple 3-day sample menu with mood-supporting nutrients. Adjust portion sizes based on your needs.
Day 1
Breakfast: Oatmeal with blueberries, walnuts, and flaxseeds
Lunch: Lentil and spinach salad with cherry tomatoes, olive oil, lemon
Snack: Yogurt with a spoonful of chia seeds
Dinner: Baked salmon, quinoa, roasted broccoli
Day 2
Breakfast: Greek yogurt parfait with mixed berries and granola
Lunch: Whole-grain wrap with hummus, roasted peppers, spinach, and canned tuna
Snack: Apple with almond butter
Dinner: Chickpea curry with brown rice and steamed greens
Day 3
Breakfast: Scrambled eggs with sautéed kale and whole-grain toast
Lunch: Quinoa bowl with black beans, avocado, corn, tomato, lime
Snack: Handful of mixed nuts and dark chocolate
Dinner: Stir-fry tofu with bell peppers, mushrooms, and mixed vegetables over soba noodles
Conclusion: Summing Up Nutrition's Impact on Mental Health
Key takeaways: actionable steps readers can start today
- Start with one or two small swaps (e.g., add a vegetable to dinner, reduce sugary drinks).
- Prioritize whole, minimally processed foods, regular meals, and a balance of protein, healthy fats, and fiber.
- Consider omega-3-rich foods, B vitamins, vitamin D, magnesium, and probiotic foods as part of a diverse diet.
- Track mood, sleep, and diet to notice improvements and patterns.
Encouragement to personalize plans and seek professional guidance
Nutrition strategies work best when adapted to your culture, budget, preferences, and medical needs. If you have moderate to severe mental health symptoms, talk to your healthcare provider before making major changes or starting supplements.
Resources and further reading on nutrition and mental health
- World Health Organization — Depression fact sheet: - SMILES trial (dietary intervention for depression):
- NIH Office of Dietary Supplements — Vitamin D, Folate, B12 fact sheets:
- The Nutrition Source, Harvard T.H. Chan School of Public Health — Healthy Eating Plate and evidence summaries:
About The Author Jaye Kelly-Johnston