Psychosomatic Disorder: Understanding Mind-Body Healing
Understanding Psychosomatic Disorders: Mind-Body Connection
Have you ever experienced a sudden, severe stomach ache just before a major public speaking event? Or perhaps you've noticed a nagging tension headache creeping in after a bitter argument with a loved one? These everyday experiences serve as the perfect foundation for understanding the mind-body connection. When psychological or emotional distress translates directly into severe physical symptoms, medical professionals refer to this as a psychosomatic disorder.
For decades, an unfair stigma surrounded this term, and patients were often dismissed with the frustrating phrase, "It’s all in your head." However, modern medicine and science confirm that these physical responses are incredibly real. Your thoughts, feelings, and fears have a direct, measurable impact on your biology.
What Are Psychosomatic Disorders?
The Overloaded Circuit: How Your Nervous System Turns Anxiety Into Physical Pain
In the rapidly evolving field of health psychology, a psychosomatic disorder is recognized as a condition where mental distress adversely affects physiological functioning. One of the most confusing hurdles for patients and doctors alike is distinguishing the difference between organic and functional illness.
An organic illness has a highly visible, easily measurable physical cause—such as a viral infection, a tumor, or a fractured bone. A functional illness, however, produces debilitating physical symptoms without an obvious structural or cellular abnormality on standard imaging or lab tests. Because the root cause is emotional or psychological strain, identifying psychogenic physical ailments can be incredibly frustrating. Patients may undergo countless MRIs, blood panels, and X-rays only to be told they are completely healthy. Yet, the pain they feel is undeniable. Acknowledging and validating this pain is the crucial first step toward meaningful healing.
The Science Behind the Symptoms
To truly grasp why our bodies hurt when our minds are troubled, we must look at the biological mechanisms of emotional distress. At the core of this phenomenon is the brain's built-in survival mechanism: the alarm system. When you face ongoing stressors—whether from a demanding job, financial worry, or relationship struggles—your body remains locked in a prolonged state of "fight or flight."
This chronic state of high alert leads to hypothalamic-pituitary-adrenal axis dysfunction. In simple terms, the HPA axis is the complex communication network between your brain and your adrenal glands. When it dysfunctions due to chronic worry, it floods your system with a continuous stream of stress hormones, primarily cortisol and adrenaline.
The long-term impact of stress on the body cannot be overstated. Constantly elevated cortisol levels can lead to high blood pressure, suppressed immunity, increased inflammation, and severe gastrointestinal disruption. These are not imaginary ailments; they are the literal, documented physical manifestations of chronic stress. To combat this cascade of hormones, focusing on autonomic nervous system regulation becomes vital. By consciously engaging the parasympathetic nervous system (the "rest and digest" mode), we can halt the flood of stress chemicals and allow the body to heal.
Can Emotional Trauma Cause Physical Pain?
A question frequently asked in doctors' offices is: can emotional trauma cause physical pain? The answer is an unequivocal yes. Unresolved trauma, deep grief, and unaddressed mental health issues frequently manifest as chronic pain, inexplicable fatigue, and severe muscle tension.
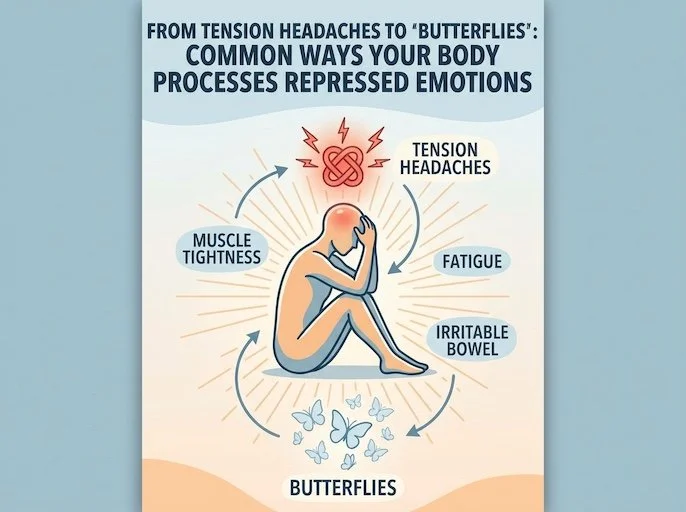
For instance, a person suffering from a psychosomatic anxiety disorder might experience terrifying heart palpitations, chest tightness, and shortness of breath that closely mimic a heart attack. When underlying emotional health is ignored or suppressed, the physical body acts as a pressure cooker. It will eventually find a way to express the emotional agony the mind refuses or is unable to process, often resulting in intense physical discomfort.From Tension Headaches to 'Butterflies': Common Ways Your Body Processes Repressed Emotions
Think of your nervous system like a steam cooker. When you push down feelings of anxiety or sadness, that trapped pressure needs a release. The biological impact of repressed emotions essentially forces your body to vent this invisible stress physically.
Medical professionals call the areas where this pressure escapes "target organs."
These are specific body parts that take the brunt of your emotional overload. While everyone is unique, psychosomatic symptoms typically strike the same vulnerable systems:
Tension headaches wrapping around your skull after difficult conversations.
Digestive flare-ups, like a churning stomach, during financial worry.
Chest tightness or racing heartbeats before entering crowded rooms.
Recognizing these warning signs is the first step toward relief. Once you see that tight shoulders can signal emotional strain, you can start managing stress-related physical pain.
Lowering the Volume: Effective Ways to Manage Stress-Induced Physical Symptoms
Since your brain controls pain intensity, your best tool for relief is teaching your nervous system to turn down the dial. Doctors call this adaptable "volume control" neuroplasticity—the brain's remarkable ability to physically rewire itself based on new habits. Embracing neuroplasticity in mind-body healing proves that your physical symptoms are not permanently stuck on high alert.
Guiding this rewiring process is beautifully achieved through cognitive behavioral therapy for somatic health. While often seen as emotional support, CBT is like physical therapy for your nervous system. It helps you catch anxious thoughts early. This awareness prevents your brain from sending unnecessary panic signals straight to your churning stomach or tense shoulders.
Immediate stress management for physical symptom relief can begin today without waiting for a doctor's appointment. Try taking slow, deep belly breaths to steady a racing heart, or purposefully drop your shoulders to release trapped muscle tension. These deliberate physical actions signal genuine safety to your brain, stopping the stress response in its tracks.
Mastering these simple adjustments finally gives you back control over your daily comfort.
Actionable Strategies: How to Manage Functional Symptoms
Learning how to manage functional symptoms effectively is the key to reclaiming your life. Achieving somatic symptom disorder recovery is rarely about one pill. It usually needs a complete, caring plan that treats the whole person. Here are several proven, actionable strategies:
Cognitive behavioral therapy for somatization: Therapy is an incredibly powerful tool for physical recovery. CBT helps patients identify and rewire catastrophic thought patterns. By easing the intense anxiety around physical symptoms, the nervous system begins to calm down. This also reduces the severity of physical pain.
Leveraging Brain Science: Believe it or not, your brain's incredible adaptability can be used to alleviate your pain. The concept of neuroplasticity and chronic symptom relief involves teaching the brain that the body is safe now. Through steady therapy and body tracking, you can change your brain’s neural pathways.
This can turn down chronic pain signals over time.
Mindfulness for stress-induced illness: Deep breathing, guided meditation, and progressive muscle relaxation are great ways to practice mindfulness. These techniques help you stay in the present moment. They send quick safety signals to your brain and naturally lower cortisol levels.
Building Holistic Health Management Strategies
Finally, true and lasting healing relies on robust holistic health management strategies. This means nourishing both your physical and emotional needs simultaneously. Prioritize a balanced, anti-inflammatory diet to support gut health.
Get restorative sleep so your brain can recover.
Engage in gentle movement like yoga, tai chi, or daily walking. These activities naturally promote endorphin release and support nervous system regulation without overtaxing a fatigued body.
The Takeaway
Living with a psychosomatic disorder can feel incredibly isolating, especially when conventional medicine struggles to provide immediate answers or solutions. However, recognizing the undeniable link between your mental state and physical symptoms is an empowering revelation. By focusing on your emotional well-being, you can break the cycle of stress and pain.
Use targeted mental health therapies.
Regulate your nervous system. Remember, your body is always listening to your mind—make sure you are speaking to it with compassion, patience, and care.